Medication & IBD: How to stay on top of your treatment
7 mins read

A new era of IBD care
The way we treat IBD has evolved significantly over the years, moving from simple symptom management to advanced therapies that target the root of inflammation. While the options can feel overwhelming, understanding how each class works helps you stay in the driver's seat of your care.
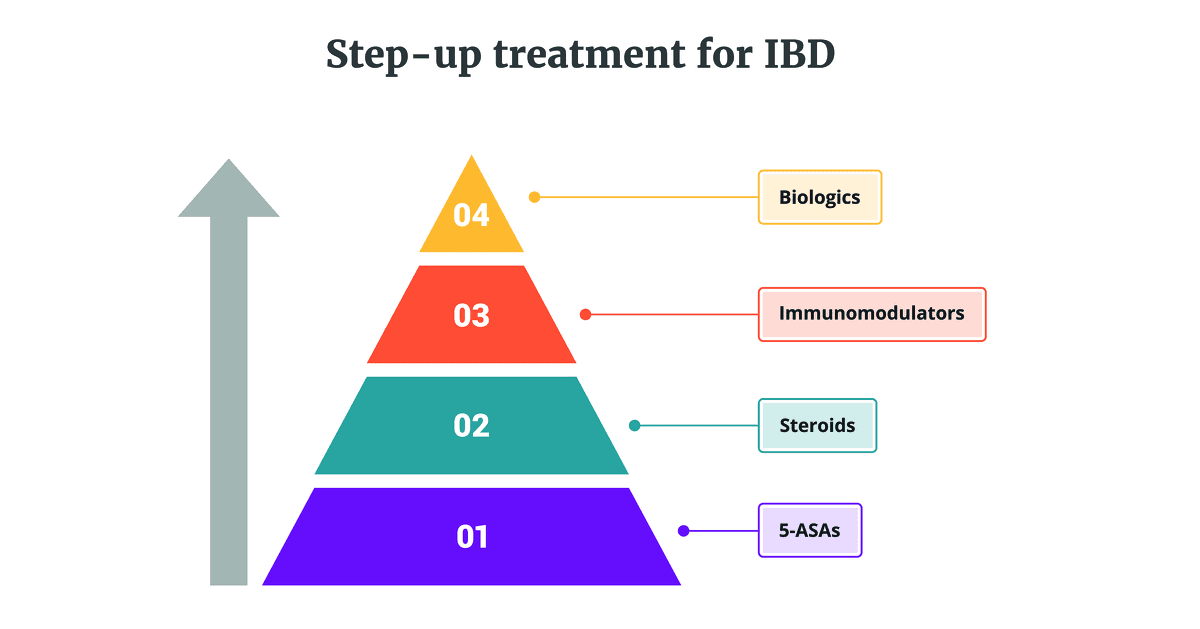
Prednisone & Steroids
For many, Prednisone is the first stop during a flare. It’s a powerful fire extinguisher designed to quickly calm inflammation and get symptoms under control. While effective for short-term relief, the goal of modern IBD care is to move toward "steroid-free remission" to avoid long-term side effects.
5-ASAs
Drugs like Pentasa, Asacol, and Salofalk (Mesalamine) are often the first line of defense for mild-to-moderate IBD. They work directly on the lining of the gut to reduce surface-level inflammation and help maintain the peace once you're feeling better.
Immunomodulators
Medications like Azathioprine or 6-MP work by dampening an overactive immune system over time. They are "slow and steady" treatments, often used to help patients stay off steroids for good and maintain long-term stability.
Biologics & Small Molecules
We’ve entered an era of advanced therapies that has given quality of life a whole new meaning. Unlike older treatments, these target specific proteins in the immune system to stop inflammation before it starts. Between biologics and small molecules like Remicade, Humira, Entyvio, Stelara, Skyrizi, Rinvoq, Omvoh, and Xeljanz, there are more ways than ever to target IBD directly.
Much like finding the right diet, finding the right medication can involve some trial and error; what works for one person might not be the right fit for another. But there is massive hope: with so many diverse options, almost everyone can find a treatment that works for their specific body.
But the prerequisite for any medication to work is adherence. And that's paramount for getting to and staying in remission with IBD.
Why perfect adherence is the goal
Having a world-class medication only works if it actually stays in your system. In the world of IBD, being "mostly" consistent with your meds isn't always enough to keep the peace.
Research shows that patients who aren't consistent with their medication are over five times more likely to experience a flare-up compared to those who stick to their schedule.
With biologics, skipping doses isn't just a temporary lapse; it can cause your immune system to develop antibodies against the medicine, making it stop working entirely.
It is tempting to feel the medicine isn't needed during those quiet periods of remission, yet skipping doses actually makes you 80% more likely to require a hospital stay. If you are using a biologic, this consistency is even more vital, as missing doses makes it three to five times more likely that the treatment will fail entirely because your body may develop a resistance to the drug.
Nearly 48% of patients find that simple forgetfulness is their biggest barrier, but embracing tools like reminder apps or the once-daily dosing that 59% of people find so helpful can transform your treatment from a daily burden into a powerful, reliable shield for your health.
This is why Chronicare lets you log your medications alongside your symptoms, so you have a complete picture of your own health over time.
How to track your medication with Chronicare
Chronicare acts as your 'digital memory,' giving you one place to record your medication history without relying on what you can recall at your next appointment. Whether you take daily pills or have a monthly infusion, you can log it all in one place.
Medication logging: Record which medications you take, at what doses, and how often — so your history is captured as it happens, not reconstructed from memory later.
Reminders & calendar sync: Set personal reminders for upcoming infusions or injections and sync them with your calendar. These are standard notification reminders — the same way you'd set a calendar alert for any appointment.
Medication timeline: Log when you started or stopped a treatment and note any reasons for changes. Over time, this builds a personal record of your IBD journey that belongs entirely to you.
Bring your own data to appointments: Your logged history is yours to share however you choose — including showing it to your doctor if you find it useful. Many patients find having their own records reduces the guesswork in conversations with their care team.





